
Estimated reading time: 5 minutes
Key Takeaways
- Rosacea is an inflammatory condition linked to immune system response, with symptoms existing on a severity continuum.
- Environmental triggers include UV light, heat, spicy foods, alcohol, stress, and changes in the microbiome.
- Overpopulation of Demodex folliculorum mites, and their associated bacteria, Bacillus oleronius, may contribute to inflammation in rosacea sufferers.
- Gut microbiome shifts, such as small intestinal bacterial overgrowth, may also be a factor in rosacea symptoms.
- Understanding rosacea requires more research on genetic predisposition and environmental factors, including potential treatments targeting the microbiome.
Rosacea: An Inflammatory Continuum
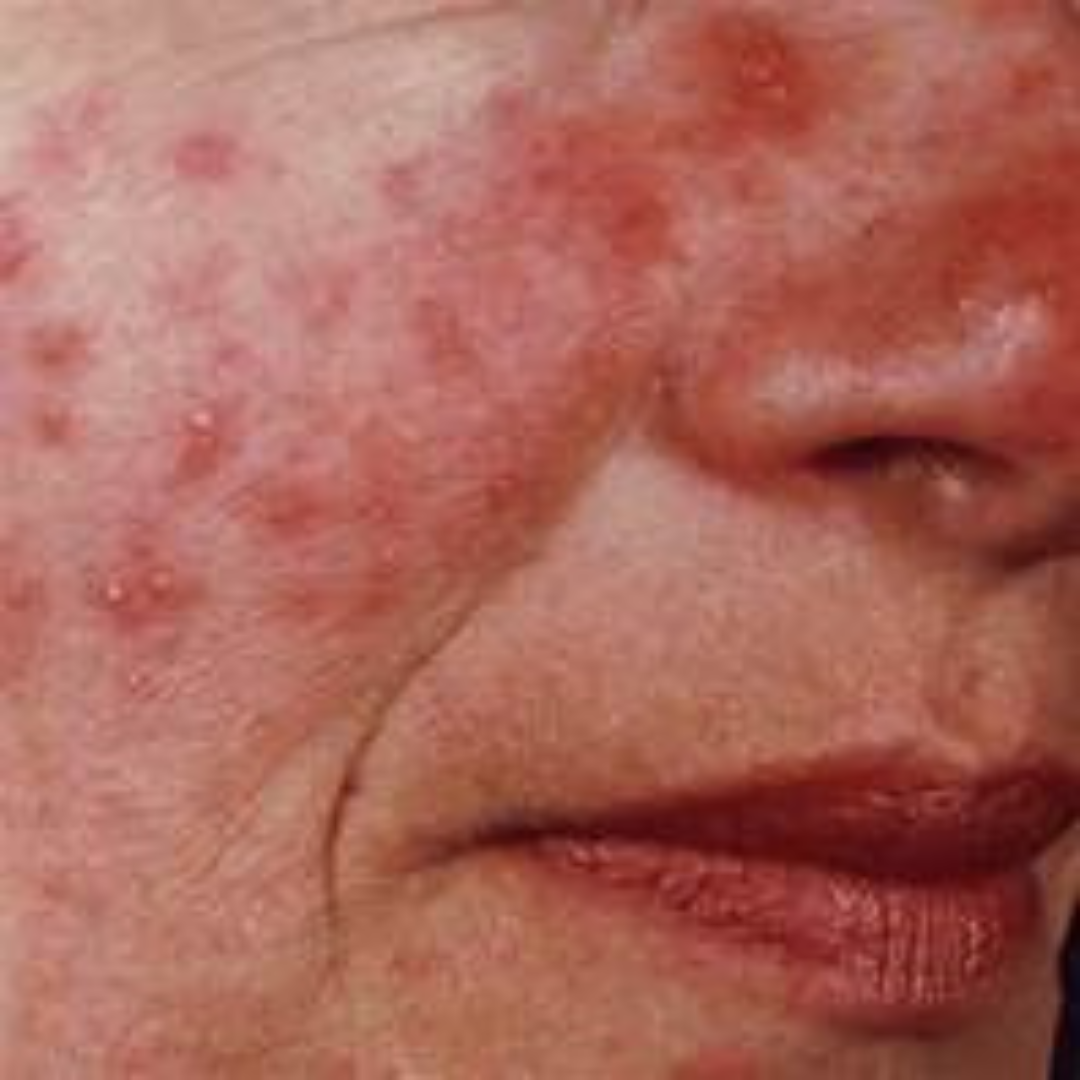
Recent scholarly writings describe rosacea as a disease of the immune system. Rosacea symptoms seem to arise from inflammation that gets out of control, triggered by environmental factors such as shifts in the microbiome. While investigation and debate continue about some particulars, there is general agreement that: (1) a number of things can trigger the inflammatory process, and (2) rosacea symptoms exist on a continuum, with some affected persons having only one or two relatively mild symptoms, and others having numerous severe symptoms. There is some thought that erythema (redness), flushing, and telangiectasias (visible blood vessels) represent the milder or earlier manifestations of rosacea, and that papules (red bumps), pustules (whiteheads) and hypertrophic (thickened skin) changes can appear if the inflammation progresses or remains high over a long period of time.2
Rosacea Triggers
Numerous environmental stimuli can spark inflammation in rosacea. These include ultraviolet light, heat, spicy foods, alcohol, stress and microbes.2 Regarding microbes, studies have shown shifts in the microbiome of the skin and gut in rosacea. Skin affected by rosacea is more likely to carry certain skin mites and certain strains of bacteria, and higher numbers of those organisms. Of particular interest in rosacea are, Staphylococcus epidermidis bacteria, the Demodex folliculorum mite, and Bacillus oleronius bacteria carried by Demodex mites.
Skin Mites and Their Associated Bacteria in Rosacea
Evidence has accumulated that Demodex mites (especially Demodex folliculorum) contribute to a cycle of inflammation in some rosacea cases. They are a normal part of healthy human microbiota, but live more commonly, and in higher density, in individuals with rosacea. Demodex mites normally control the immune system of their human host to make it tolerant of their presence.2 It seems, however, that these mites can proliferate and become densely populated at some point in rosacea, triggering the immune system to respond with inflammation. It is not yet settled whether mite proliferation triggers rosacea, or whether the conditions of early rosacea favor mite proliferation, which then leads to a cycle of increased rosacea symptoms.
In microscope examination of skin tissue, Demodex mites have been found in 63% of people with erythema and telangiectasia of rosacea, 85% to nearly 100% of those with papules and pustules of rosacea, and 100% of those with hypertrophic rosacea characterized by thickened overgrown skin (typically seen as a bulbous nose).1,5 For context, the global pooled prevalence of human Demodex mites is estimated at 35%, with the highest prevalence observed in the South-East Asia Region at 44%.4 Demodex mites carry Bacillus oleronius bacteria, and some have theorized that it is the bacteria, rather than the mites, that are most responsible for stimulating an inflammatory reaction in rosacea.3
Shifted Gut Microbiome in Rosacea?
A small study of 63 rosacea patients showed that about half of them also had small intestinal bacteria overgrowth, or SIBO.6 It was published as a letter in the Journal of the American Academy of Dermatology, and asserted that 46 percent of these patients reported marked improvement of their rosacea symptoms after localized treatment for SIBO.6 This merits further study, particularly because we now know that the gut plays a starring role in immune function.
Certainly, more progress remains in our understanding of rosacea. What we know for now fits the mold of many other diseases: It looks be a case of genetic predisposition, with disease expression (symptoms and the severity of them) shaped by multiple environmental influences.
Next Up? How to Tackle Shifts in the Skin Microbiome. Hint: Start with things you apply to the skin rather than things you swallow and ingest. Ivermectin cream, permethrin, and skincare with high-quality tea tree oil all have at least some evidence of effectiveness against Demodex mites and Bacillus oleronius.
Citations
- Cribier, B. (2013). Rosacea under the microscope: Characteristic histological findings. Journal of the European Academy of Dermatology and Venereology, 27(11), 1336–1343.
- Forton, F. M. N. (2020). The pathogenic role of Demodex mites in rosacea: A potential therapeutic target already in erythematotelangiectatic rosacea? Adis Journals. https://doi.org/10.6084/m9.figshare.13042940.v1
- Lacey, N., Delaney, S., Kavanagh, K., & Powell, F. C. (2007). Mite-related bacterial antigens stimulate inflammatory cells in rosacea. British Journal of Dermatology, 157(3), 474–481.
- Maleki, B., Haghshenas, N., Rezaei-Tavirani, M., Ahmadzadeh, A., Abolghazi, A., & Robati, R. M. (2025). Global prevalence of human Demodex mite: A systematic review and meta-analysis. Acta Tropica, 268, 107693. https://doi.org/10.1016/j.actatropica.2025.107693
- Perrigouard, C., Peltre, B., & Cribier, B. (2013). A histological and immunohistological study of vascular and inflammatory changes in rosacea. Annales de Dermatologie et de Vénérologie, 140(1), 21–29.
- Weinstock LB, Steinhoff M. Rosacea and small intestinal bacterial overgrowth: prevalence and response to rifaximin. Journal of the American Academy of Dermatology 2013;68:875-876.
- Whitfeld, M., Gunasingam, N., Leow, L. J., Shirato, K., & Preda, V. (2011). Staphylococcus epidermidis: A possible role in the pustules of rosacea. Journal of the American Academy of Dermatology, 64(1), 49–52.

Shannon L. Johnson NP-C
Founder & Formulator, MeridaSKIN
Shannon is a nationally-certified Family Nurse Practitioner with twenty years of internal medicine experience. She holds Bachelor's degrees from the University of Pennsylvania and Simmons University, a Master's degree from Simmons University, and completed a post-graduate program at the University of Massachusetts Boston. She has worked in primary, emergency and urgent care settings. Ms. Johnson has precepted nurse practitioner students for clinical rotations, mentored new graduate nurse practitioners, and served as adjunct faculty teaching graduate-level pathophysiology and advanced pharmacology. She completed courses in cosmetic formulating to solve her own skin struggle with rosacea, ultimately formulating and founding MeridaSKIN. Shannon enjoys spending time in the beautiful outdoors with her husband and kids.

Recent Comments