Key Takeaways
- Effective treatment of rosacea is hampered by outstanding questions about its causes, but inflammation from Demodex mites and certain bacteria seems to play a key role.
- Tea tree oil for rosacea shows promise, as it reduces inflammation and kills Demodex mites.
- Research indicates tea tree oil effectively targets bacteria like B. oleronius and S. epidermidis, potentially alleviating rosacea issues.
- Patients may prefer tea tree oil to medical therapy due to its accessibility, efficacy, and safety.
- Safety precautions: never swallow tea tree oil, and only use it in carefully made products to minimize allergic reactions.
Challenges in Treating Rosacea
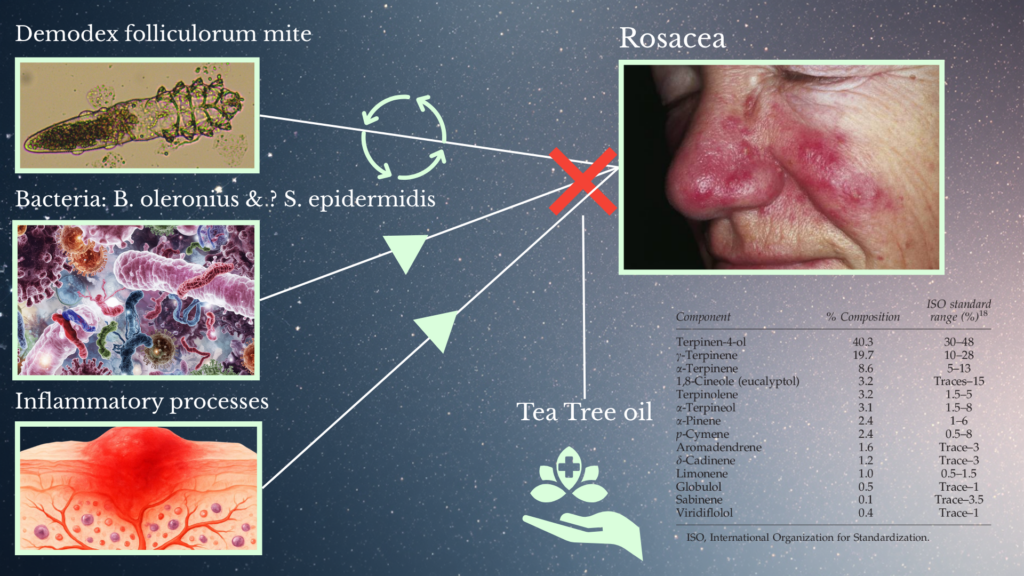
Rosacea is difficult to treat because it is not well understood. Researchers have identified many possible factors, but the explanation remains unclear. They do agree that rosacea is characterized by out-of-control inflammation. There is also mounting evidence that the inflammation is caused by overabundance of the parasitic Demodex folliculorum skin mite and certain bacteria.
Things That May Cause Rosacea
According to the National Rosacea Society, “evidence appears to be mounting that an overabundance of Demodex may possibly trigger an immune response in people with rosacea, or that the inflammation may be caused by certain bacteria associated with the mites.” (National Rosacea Society, 2026 March 26, Causes of Rosacea: Demodex Mites & Microbes | Rosacea.org). Most humans carry Demodex folliculorum mites in facial hair follicles, but people with rosacea have more of them (Chang & Huang, 2017; Lacey et al., 2007). An analysis of the relationship between Demodex and rosacea by Forton (2012) concluded that the inflammatory process of papulopustular rosacea appears to be a consequence of Demodex proliferation, and not the other way around. Wei et al. (2024) performed a comprehensive literature review, leading them to suggest that rosacea favors the growth of Demodex, and overgrowth of Demodex exacerbates the symptoms of rosacea, creating a vicious cycle.
There is evidence to suggest that a Demodex-carried bacteria sparks the inflammation, rather than the mite itself. Bacillus oleronius is a bacterium found in the mite. A study by Lacey et al. (2007) showed that B. oleronius triggered inflammation in 79 percent of rosacea patients. Another small study implicated a different bacterial species, Staphylococcus epidermidis, finding pure growths of it in the pustules of rosacea (Whitfield et al., 2011).
Things That Should Help Rosacea
From what we know so far about rosacea, it should improve with things that: (1) lower inflammation, (2) reduce or eliminate the Demodex folliculorum mite, and (3) kill B. oleronius and S. epidermidis bacteria. Indeed, studies show improvement with topical ivermectin, which is anti-inflammatory and kills arachnids like the Demodex mite. Some rosacea cases also improve with topical metronidazole, which is anti-inflammatory, and with the tetracycline antibiotics, which are anti-bacterial. However, none of the currently available prescription medications perform all three functions. Enter: tea tree oil.
Tea Tree Oil as an Anti-Inflammatory in Rosacea
Numerous studies demonstrate anti-inflammatory effects of tea tree oil (TTO) and show that it affects a range of immune responses (Carson et al., 2006). Many signaling chemicals are involved in inflammation. Carson et al. (2006) show that TTO decreases a variety of them, including: tumor necrosis factor alpha (TNF-α), interleukin-1β (IL-1β), IL-8, IL-10, prostaglandin E2 and reactive oxygen species. Koh et al. (2002) show that it also reduces histamine-induced inflammation. The important thing is that this reduction in inflammatory chemicals leads to symptom improvement. That is, that the person actually feels better. Though people using TTO products do seem to experience improvement in their rosacea symptoms, it is difficult to determine how much of the improvement is due to anti-inflammatory effect alone, because TTO also has antimicrobial actions that can lead to improvement.
Tea Tree Oil to Combat Demodex folliculorum in Rosacea
Tea tree oil (TTO) is effective in killing Demodex folliculorum. A split face study showed that tea tree oil combined with permethrin 2.5% in gel was safe and effective in reducing Demodex mite counts and the inflammatory effects of rosacea (Ebneyamin et al., 2020). The side of the face treated with permethrin and tea tree oil improved to a significant degree. The side of the face treated with placebo gel did not. Naturally, the next question is whether the improvement came from permethrin, tea tree oil, or the combination.
That question is addressed in a study by Yürekli & Botsali (2022), which compared survival time of Demodex folliculorum mites on exposure to permethrin 5%, six different concentrations of TTO, and a control oil. It showed that Demodex mites died more quickly on exposure to TTO than on exposure to the control oil. Importantly, the survival time showed a dose-related pattern. That is, the mites died more quickly with each step up in the concentration of TTO. It also showed that survival time was roughly the same for TTO 25% and permethrin 5%. How does TTO work against Demodex mites? The antiparasitic effect of TTO is partly attributed to the anticholinesterase activity of several of its components, which can cause deadly muscle contraction and paralysis of the parasite (Bezabh et al., 2022).
Tea Tree Oil to Limit B. oleronius and S. epidermidis in Rosacea
Tea tree oil (TTO) has broad spectrum antimicrobial effects. Carson et al. (2006) summarize the susceptibilities of a broad range of bacteria to tea tree oil. Most of the tested bacteria died (were susceptible) at a TTO concentration of 1% or less. This included susceptibility of a Bacillus species and of S. epidermidis. That same paper confirms that TTO compromises the structural and functional integrity of bacterial cell membranes through a variety of effects. This variety of effects makes it unlikely that micro-organisms will develop resistance to tea tree oil. Carson et al. (2006) wrote, “It is likely that the multicomponent nature of TTO may reduce the potential for resistance to occur spontaneously, since multiple simultaneous mutations may be required to overcome all of the antimicrobial actions of each of the components.”
Safety When Using Tea Tree Oil for Rosacea
- Never swallow tea tree oil (TTO). It is toxic if ingested.
- Do not apply undiluted (pure) TTO due to increased risk of contact allergy. Most allergic reactions to TTO are due to application of pure oil. The prevalence of positive patch test results range from 0.1-3.5% in routine testing (de Groot & Schmidt, 2016).
- Only use a TTO product if unexpired and properly stored. The chemical composition of the oil changes as oxidation occurs with age and exposure to air. Oxidation of the oil increases its allergic potential (de Groot & Schmidt, 2016). Carson et al. (2006) noted that “Light, heat, exposure to air, and moisture all affect oil stability, and TTO should be stored in dark, cool, dry conditions, preferably in a vessel that contains little air.”
Tea Tree Oil vs. Topical Prescriptions for Rosacea
Tea tree oil (TTO) is a complex botanical product with potential benefits for skin suffering with inflammation and disease-causing bacteria and parasites. Several things about TTO lend appeal. First, TTO products are accessible without a prescription or medical visit. Second, TTO seems to compare well to prescription treatments in terms of effectiveness for rosacea. Lam et. al (2020) compared tea tree oil with pharmacological treatments for rosacea and found that TTO was the most effective in managing the disease, followed by metronidazole, ivermectin and permethrin. Finally, topical TTO has a safety profile that compares favorably with the available prescription treatments for rosacea. The topical prescriptions for rosacea all report the possibility of application site reactions such as burning, itching, stinging, dryness and redness. The likelihood of these reactions varies from one medication to another, but the observed rate of contact allergy with pure undiluted TTO is not out of line with the prescription topicals.
It is important to note that tea tree oil, along with active ingredients in topical drugs, are only as good as their carrier vehicle (e.g., cream, gel, foam). If the carrier itself is allergenic or irritating to skin, its harms may outweigh the benefits of the active it delivers.
Conclusion
Compared to the available prescription treatments for rosacea, products containing high quality tea tree oil can be more easily accessible, yield more improvement, have fewer unpleasant side effects, and cost less per month of use. When incorporated into carefully formulated skincare products, tea tree oil is a useful addition to prescription therapy for rosacea. Some may even find it preferable as the first step in addressing rosacea symptoms.
References A-F
Bezabh, S. A., Tesfaye, W., Christenson, J. K., Carson, C. F., & Thomas, J. (2022). Antiparasitic activity of tea tree oil (TTO) and its components against medically important ectoparasites: A systematic review. Pharmaceutics, 14(8), 1587.
Carson, C. F., Hammer, K. A., & Riley, T. V. (2006). Melaleuca alternifolia (tea tree) oil: a review of antimicrobial and other medicinal properties. Clinical microbiology reviews, 19(1), 50-62.
Chang, Y. S., & Huang, Y. C. (2017). Role of Demodex mite infestation in rosacea: a systematic review and meta-analysis. Journal of the American Academy of Dermatology, 77(3), 441-447.
de Groot, A. C., & Schmidt, E. (2016). Tea tree oil: contact allergy and chemical composition. Contact dermatitis, 75(3), 129-143.
Ebneyamin, E., Mansouri, P., Rajabi, M., Qomi, M., Asgharian, R., & Azizian, Z. (2020). The efficacy and safety of permethrin 2.5% with tea tree oil gel on rosacea treatment: A double‐blind, controlled clinical trial. Journal of cosmetic dermatology, 19(6), 1426-1431.
Forton, F. M. N. (2012). Papulopustular rosacea, skin immunity and Demodex: pityriasis folliculorum as a missing link. Journal of the European Academy of Dermatology and Venereology, 26(1), 19-28.
References K-Z
Koh, K. J., Pearce, A. L., Marshman, G., Finlay‐Jones, J. J., & Hart, P. H. (2002). Tea tree oil reduces histamine‐induced skin inflammation. British Journal of Dermatology, 147(6), 1212-1217.
Lacey, N., Delaney, S., Kavanagh, K., & Powell, F. C. (2007). Mite‐related bacterial antigens stimulate inflammatory cells in rosacea. British Journal of Dermatology, 157(3), 474-481.
Lam, N. S. K., Long, X. X., Li, X., Yang, L., Griffin, R. C., & Doery, J. C. (2020). Comparison of the efficacy of tea tree (Melaleuca alternifolia) oil with other current pharmacological management in human demodicosis: A Systematic Review. Parasitology, 147(14), 1587-1613.
National Rosacea Society. (2026, March 26). Causes of Rosacea: Demodex Mites and Microbes. National Rosacea Society website. Causes of Rosacea: Demodex Mites & Microbes | Rosacea.org
Wei, F., Li, L., Kong, Y., Yan, X., Varghese, K. J., Zhang, S., … & Chen, H. (2024). Evidence for the clinical association between demodex and rosacea: a review. Dermatology, 240(1), 95-102.
Whitfeld, M., Gunasingam, N., Leow, L. J., Shirato, K., & Preda, V. (2011). Staphylococcus epidermidis: a possible role in the pustules of rosacea. Journal of the American Academy of Dermatology, 64(1), 49-52.
Yurekli, A. & Botsali, A. (2022). The comparative in vitro killing activity of tea tree oil versus permethrin on Demodex folliculorum of rosacea patients. Journal of cosmetic dermatology, 21(5), 2268-2272.

Shannon L. Johnson NP-C
Founder & Formulator, MeridaSKIN
Shannon is a nationally-certified Family Nurse Practitioner with twenty years of internal medicine experience. She holds Bachelor's degrees from the University of Pennsylvania and Simmons University, a Master's degree from Simmons University, and completed a post-graduate program at the University of Massachusetts Boston. She has worked in primary, emergency and urgent care settings. Ms. Johnson has precepted nurse practitioner students for clinical rotations, mentored new graduate nurse practitioners, and served as adjunct faculty teaching graduate-level pathophysiology and advanced pharmacology. She completed courses in cosmetic formulating to solve her own skin struggle with rosacea, ultimately formulating and founding MeridaSKIN. Shannon enjoys spending time in the beautiful outdoors with her husband and kids.

Recent Comments